Statins
Dear reader,
A question which I often get from patients is —
‘Can heart artery blockages be reversed? If yes, what can I do to reduce my heart artery blockages besides coronary angioplasty and stenting?’
With the current data, we now have some answers to these questions.
There are a few factors which have been shown to reduce heart attacks and also possibly reduce blockages. Some examples include certain medications and diet.
Firstly, we will talk about an important agent that reduces heart attacks and has been shown to be able to reduce blockages in certain situations: Statins.
Statins are a type of medication that originated from a fungus present naturally in the environment. It was a great discovery then, as it was the first treatment that significantly reduced bad cholesterol levels. Subsequently, other synthetic statins were produced with modifications to the original chemical structure. These had good results in reducing cardiac events and in an early trial, treatment with a statin was shown to reduce death from heart disease by 42%.1
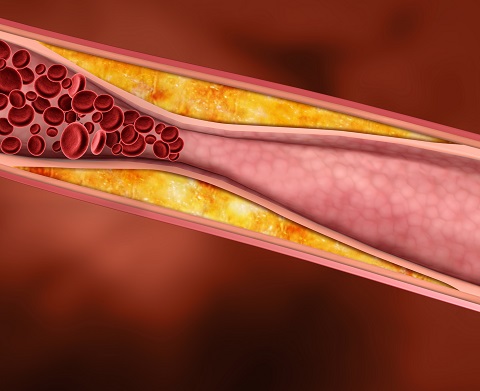
Statins significantly reduce bad cholesterol (also called LDL) levels, with varying effects depending on the individual but generally are effective therapies in reducing LDL. When there is excessive LDL circulating in the blood, cholesterol tends to become deposited in the inner lining of arteries. Inflammatory cells are then attracted to these deposits and act on them, forming plaque, which are deposits in arteries that can cause blockages. In addition, these deposits can break apart abruptly and set off a cascade of events in the blood vessel causing a blood clot to form rapidly, choking off blood supply completely and resulting in a heart attack. Hence, reducing LDL lowers heart attack risk.
Statins also have an anti-inflammatory effect in the blood vessel, stabilising the unstable plaque, reducing the likelihood of the plaque breaking apart, thereby reducing the risk of a heart attack.
The more LDL is lowered by using statins, the greater the reduction in heart attacks and stroke. Data analysed from 26 statin studies showed that every additional 1 mmol/L reduction of LDL by statin treatment reduced the incidence of strokes/heart attacks by 22% over a median of 5 years of treatment with statin.2 The effect was less during the first year of treatment, followed by a consistent 22-24% reduction in events of stroke or heart attack per 1 mmol/L reduction in LDL during each subsequent year of treatment.3
Statins have been shown to be able to reduce the amount of plaque in arteries. When LDL was lowered to less than 2.1 mmol/L, particularly if it was lowered to 1.8 mmol/L or less, plaque reduction would be more likely to occur.4
Lastly, many think this very useful agent can cause cancer, or liver or kidney problems.
Fact: Statins do not cause cancer or kidney problems. The incidence of liver problems with statins are rare, at less than 1%. Even if it occurs, often times these only cause mild derangement in liver enzymes, and if so, the statin can be continued under your doctor’s advice and monitoring, without any significant adverse effects to the function of the liver.
Clin Asst Prof Huang Zijuan is a Consultant Cardiologist with sub-specialty interests in Preventive Cardiology and Cardiac Rehabilitation, Nuclear Cardiac Imaging and Cardiac CT. Read more on her profile.
References:
1. Wright RA, Flapan AD, McMurray J, et al. Scandinavian simvastatin study (4S). Lancet. 1994;344(8939-8940):1765-1768. doi:10.1016/S0140-6736(94)92906-8
2. Baigent C, Blackwell L, Emberson J, et al. Efficacy and safety of more intensive lowering of LDL cholesterol: a meta-analysis of data from 170 000 participants in 26 randomised trials. Lancet. 2010;376(9753):1670. doi:10.1016/S0140-6736(10)61350-5
3. Collins R, Reith C, Emberson J, et al. Interpretation of the evidence for the efficacy and safety of statin therapy. Lancet (London, England). 2016;388(10059):2532-2561. doi:10.1016/S0140-6736(16)31357-5
4. Li Y, Deng S, Liu B, et al. The effects of lipid-lowering therapy on coronary plaque regression: a systematic review and meta-analysis. Sci Rep. 2021;11(1). doi:10.1038/S41598-021-87528-W
Tags:
;
;
;
Coronary Artery Disease / Coronary Heart Disease;Heart Attack (Chest Pain);Coronary Angioplasty;
News Article;Internal;
National Heart Centre Singapore;
National Heart Centre Singapore;
Article;
Stories from the Heart (NHCS);
;
;
National Heart Centre Singapore;
;
Stories from the heart
