Singapore General Hospital will NEVER ask you to transfer money over a call. If in doubt, call the 24/7 ScamShield helpline at 1799, or visit the ScamShield website at www.scamshield.gov.sg.
We’d love to hear from you! Rate the SGH website and share your feedback so we can enhance your online experience and serve you better. Click here to rate us
Pregnant women who postpone their COVID-19 vaccination risk complications to themselves and their unborn foetuses if they catch the virus before delivery, as the experience of these two mothers show.
Ms Yvonne Khoo
nearly lost her life
when she caught
the COVID-19 virus
in her 25th week of pregnancy.
Unvaccinated, Ms Khoo had
severe respiratory failure when
she was admitted to Singapore
General Hospital (SGH) in late
October last year.

(Photo: Ms Yvonne Khoo)
At SGH’s intensive care unit (ICU), she immediately had a breathing tube connected to a machine to help her breathe. Even with the ventilator, “her oxygen level was very, very low,” said Dr Sewa Duu Wen, Senior Consultant, Department of Respiratory and Critical Care Medicine, SGH. He is also Director, Medical ICU.
Ms Khoo’s oxygen level had plunged to 70 per cent from the normal 95 to 100 per cent. Oxygen levels of under 90 per cent are considered a clinical emergency. “Her condition was precarious. Our consideration was how to save the mother, even as we also wanted to save the baby,” Dr Sewa said.

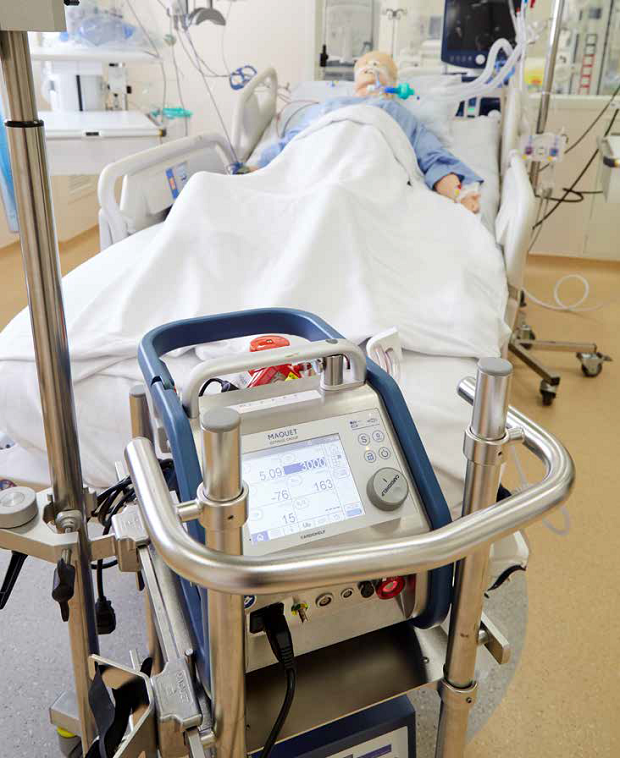
<<Dr Sewa Duu Wen (with Nurse Clinician Anwen Chan Shi) demonstrates on a mannequin the setting up of the ECMO machine, which takes over the functions of a patient’s lungs and heart to allow the infected lungs to recover.>>
Meanwhile, a large team of specialists — respiratory, obstetrics, anaesthesiology, intensive care, infectious diseases, neonatal care — was quickly assembled, and put on standby and on high alert. “Everyone had to come together literally at the snap of the finger,” said Dr Tan Wei Ching, Senior Consultant, Department of Obstetrics & Gynaecology (O&G), SGH.
One option the team considered was to deliver the baby immediately to improve
Ms Khoo’s chances of survival. For Dr Tan, a key consideration was the baby’s prematurity. “Should we deliver baby at just 25 weeks?” she said, noting that issues like safe transfer of Ms Khoo to the operating theatre (OT) with equipment necessary for a caesarean section and other emergencies, or delivery at the ICU, also had to be addressed. Ms Khoo’s condition was deteriorating rapidly. Her COVID-19 infection was complicated not just by her pregnancy, but also an underlying kidney condition. Compared to other people, pregnant women have a greater chance of developing severe complications if they are infected with the virus.
Treatment for Ms Khoo’s kidney disease had also weakened her immune system. She was thus more prone to a very severe form of COVID-19 infection, said Dr Sewa. Still, the team decided to let Ms Khoo’s baby develop further in the womb. To give mother and baby the best chance of survival, Ms Khoo was deeply sedated and put on extracorporeal membrane oxygenation (ECMO) therapy.
ECMO takes over the function of the patient’s lungs and heart, allowing the infected lungs time to recover. Blood is taken out through the big veins, passed through the artificial ECMO lung, where carbon dioxide is taken out and oxygen added before being pumped back into the patient for circulation through the body. For Ms Khoo, getting enough oxygen would also help prevent her foetus from suffering oxygen deprivation.
Ms Khoo spent six days supported by ECMO, and another day on the ventilator before she was able to breathe well on her own. Not long into her recovery, Ms Khoo began to have labour pains and delivered her son at 27 weeks. Although still very early, the extra weeks spent in the womb to develop naturally increased the baby’s survival odds, said Dr Tan.
Although baby Yohanne weighed just 789g at birth, he was unaffected by his mother’s COVID-19 infection and ECMO therapy, and was cared for at SGH’s neonatal high-dependency ward. Ms Khoo, however, experienced chest pains, difficulty in breathing, and trembling hands even after recovery. She also needed physical and occupational therapy to relearn daily activities like walking, writing and getting out of bed.
“I don’t think pregnant mothers would want to go through what I did. I had no choice but to birth my baby three months early and let my baby suffer,” said Ms Khoo. The 37-year-old described her one-month stay in isolation at SGH without her family by her side as “not an easy road”. During her illness, the now-mother of four worried about dying and leaving her children behind.
Looking back, she wished she had been inoculated early, instead of considering having one only during her second trimester of pregnancy. “If I had been vaccinated, I think my body would have been able to fight the virus,” Ms Khoo said.
Like Ms Khoo, Ms Vanessa Rickard also became infected with COVID-19 during her pregnancy. Her experience was not as harrowing, but the loneliness and fears she experienced in hospital isolation made her determined to encourage other pregnant women about early vaccination. Her family was not able to visit her; furthermore, her husband, elder son and helper also contracted the coronavirus.

(Photo: Ms Vanessa Rickard)
When Ms Rickard, then 36, became pregnant during the early days of the pandemic, little information was available about the efficacy and safety of the vaccine on the unborn foetus. Mothers are understandably concerned about how the vaccine might affect their foetus, such as the potential risks of infection, foetal abnormalities or preterm labour, said O&G’s Dr Tan.
Indeed, Ms Rickard had many of these concerns. “I thought I would just wait till I gave birth and get vaccinated after that. I wasn’t sure what effects the vaccine would have on my baby,” she said.
It was only in the second half of 2021 that studies started becoming available showing that vaccination was safe for pregnant women, and that it does not increase the risks of miscarriage, preterm labour, or small, growthretarded babies. “In fact, it is COVID-19 itself that will increase the risk of pregnancy-related complications if the mother gets very sick,” said Dr Tan.
Ms Rickard tested positive for COVID-19 and was admitted to SGH’s isolation ward in mid-August. Although her symptoms were relatively mild — runny nose, dry cough, fatigue and loss of smell — she was already in her ninth month of pregnancy. A week later, she felt labour pains and delivered her baby son. She was the first patient to give birth in an SGH isolation ward.
At the time, Singapore had begun seeing a marked increase in community COVID-19 cases. At SGH, the number of pregnant women infected with COVID-19 rose in tandem — from none in July to more than 10 in August and September, said Dr Benjamin Cherng, Senior Consultant, Department of Infectious Diseases, SGH.
“Almost all were unvaccinated, and a few were partially vaccinated. Vaccination rates among this cohort of pregnant women who came through SGH then were extremely low,” said Dr Cherng.
The vaccine has since been shown to be safe for both mother and foetus. “The benefits [of vaccination] certainly outweigh the risks of COVID-19 and its complications,” said Dr Cherng.
Interaction between newborn babies and COVID-positive mothers has not been shown to cause an increase in the incidence of neonatal COVID-19 infection, but Ms Rickard chose to be separated from her son for two-and- a-half weeks after delivery. She saw him only via video call.
As with new mothers who have had their vaccination, the breast milk of COVID-positive mothers is also safe and beneficial for babies. Moreover, the Ministry of Health (MOH) said the breast milk of vaccinated mothers may help protect babies from COVID-19 due to antibodies in the breast milk.
“Initially, when the pandemic started, breast milk was not given to babies, but now, the evidence is pretty clear that breast milk is the best and gives protection for the baby,” said Dr Sridhar Arunachalam, Consultant, Department of Neonatal and Developmental Medicine, SGH. The hospital has also been encouraging mothers to breastfeed their babies.
MOH added that no vaccinerelated side effects have been reported in the babies breastfed by mothers who received the vaccine while breastfeeding. As infections in Singapore and elsewhere are climbing again with the advent of the Omicron variant, the need to be vaccinated is ever more urgent.
“Even one dose [of a vaccine] before delivery is better than nothing,” said Dr Tan.
Get the latest updates about Singapore Health in your mailbox! Click here to subscribe.
Stay Healthy With
Outram Road, Singapore 169608
© 2025 SingHealth Group. All Rights Reserved.



















