Study aims to improve women’s fertility, metabolic and mental health, as well as develop healthy habits for their children.
A woman’s psychological wellbeing and metabolic health are fast becoming health concerns for both mother and child. These aspects have impact on one’s risk for chronic conditions such as obesity and heart conditions, from pre-conception till long after the child is born. A new care model aims to improve these issues through early intervention, even before a woman becomes pregnant. The Healthy Early Life Moments in Singapore (HELMS) study was launched by KK Women’s and Children’s Hospital (KKH) in April 2022 with the Lien Foundation and Singapore-based gut microbiome company AMILI.

Rapid societal changes have transformed Singapore within a single generation, said Professor Fabian Yap (above), Head of Endocrinology Service, Department of Paediatrics, KKH. “Along with this progress, a profound change of how we expend energy and take in calories has set the stage for an obesity pandemic,” he said. “Society has shifted from scarcity to excess, under-nutrition to over-nutrition, communicable to non-communicable diseases and from mortality to morbidity. We now have more, eat more and live longer. Yet, we have less time to prepare for pregnancy and have acquired less healthy habits and behaviours.”

Conventionally, care for the woman starts after she gets pregnant, said Professor Jerry Chan (above), Director, SingHealth Duke-NUS Maternal and Child Health Research Institute.
“However, interventions targeted at this stage of pregnancy have failed to improve outcomes for conditions such as gestational diabetes and preterm births, among others. Early intervention in the preconception phase has shown promise in some overseas trials, and HELMS has been designed to intervene as early as possible to maximise benefits for the mother and her child.”
The aim is to prevent metabolic disease from developing or progressing in families, explained Prof Yap. “HELMS presents an opportunity to break the vicious cycle of disease and chronic conditions in future generations. It adopts a life course approach to optimise health outcomes for women and their children during a crucial stage of life. With early intervention to establish the right habits and conditions prior to conception, we can improve the chances of women getting pregnant and minimise the risk of pregnancy complications.”
Among pregnant women, six per cent run the risk of pregnancy-induced hypertension (PIH), pre-eclampsia or eclampsia, which is a condition that can lead to seizures and even coma. Also, 15 to 18 per cent of pregnant women are diagnosed with gestational diabetes mellitus.
An unhealthy metabolic status can reduce the chance of conception by up to 60 per cent. Correspondingly, improved metabolic health markers, coupled with mental well-being, can result in improved fertility, said Prof Chan. Also, women with symptoms of depression or anxiety were found to have greater probabilities of experiencing female sexual dysfunction, which in turn could delay conception.
Depression and anxiety that exist in preconception persist during and after pregnancy, thereby predisposing the expectant mother to pregnancy complications. There is also strong correlation between maternal anxiety and the risk of childhood psychological and cognitive difficulties that can extend through the pre-school ages and beyond. Statistics show that nearly 40 per cent of mothers exhibit depressive symptoms during pregnancy. These symptoms strongly continue across pregnancy and into the early postnatal period.
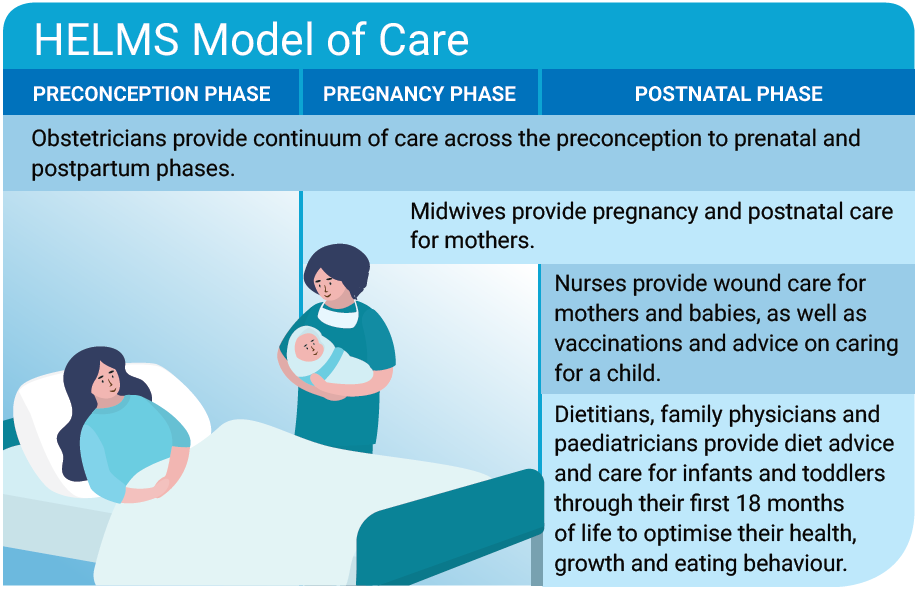
Healthcare staff across various disciplines — obstetrics, neonatology, paediatrics, nursing, dietetics and midwifery — come together under HELMS to offer information and evidenceinformed care, from preconception through pregnancy and the postnatal phase.
Study plan
Over the next four years, HELMS will study 500 overweight women from preconception readiness through two years of postnatal care of the mother and child. “Participants will receive a comprehensive package to optimise fertility, reduce risk of gestational diabetes, restore physical and mental vitality post-delivery and give their baby a head start in life,” said Prof Chan.
HELMS is available on an electronic platform, which will eventually be available on a mobile health platform called e-HELMS. Participants on e-HELMS can access their health information via their mobile devices and a wearable accessory that helps keep track and learn the impact of daily sleep patterns, activity levels, dietary choices and readiness for the next day. There is also a function for remote healthcare support via e-HELMS.
Couples planning to conceive and interested to participate in HELMS can email helms@kkh.com.sg or call 8044 4556 (Monday to Friday, 9.00am to 5.00pm) to find out more.
Get the latest updates about Singapore Health in your mailbox! Click here to subscribe.
Tags:
;
;
;
;
News Article;
;
SingHealth;KK Women's and Children's Hospital;
Article;
Singapore Health;
;
;
;
;
Singapore Health
