An arrhythmia refers to irregular or abnormal heart rhythm – either the heart rate is beating too fast or slow, or the heart rhythm is erratic with too early or premature heart beats. This happens when the electrical signals coordinating the heart beats do not work properly.
By Dr Julian Tay Cheong Kiat, Associate Consultant, Department of Cardiology
Arrhythmias can be broadly classified into four main types: tachycardia, bradycardia, premature (extra) beats, and atrial fibrillation/ flutter.
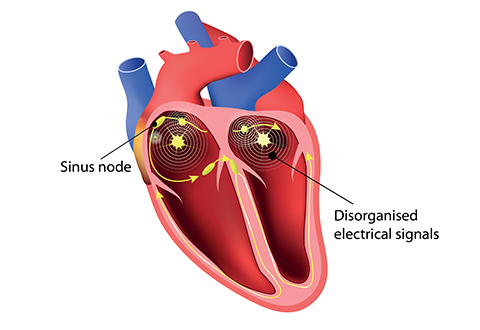
Cardiac arrhythmia - disorganised electrical signals that happen in the chamber of the heart.
Tachycardia
Tachycardia is a heart rhythm disorder where the heart beats at very high rate of 100 times a minute. It can either begin in the top chamber of the heart (atria) – known as supraventricular tachycardia (SVT) or from the bottom chamber of the heart (ventricles) – ventricular tachycardia (VT).
In SVT, the heart may suddenly beat faster and then slow down abruptly due to “short-circuits” within the heart. This type of arrhythmia is usually not life-threatening and occurs in both the young and old but causes bothersome symptoms at times.
On the other hand, VT can be life-threatening as it can degenerate into more dangerous arrhythmia such as ventricular fibrillation (VF) and generally requires immediate medical attention. This type of arrhythmia usually occurs in patients with pre-existing heart condition or cardiac history such as heart attack (myocardial infarction), heart muscle inflammation (myocarditis) and weakness (cardiomyopathy).
Bradycardia
This condition refers to heart rate that is slower than normal, at fewer than 60 beats a minute. It can be due to a problem with the sinus node – our own natural “pacemaker” or the conduction system – the electrical wiring system that conducts electrical signals within the heart to facilitate normal heartbeat. Generally, these signals can sometimes be blocked or slow down due to aging but in other situations, the disrupted signals can occur due to diseased processes or medications. Any slowing or block in the sinus node or conduction system can lead to heart failure or fainting with bodily injuries in some cases.
Extra beats
These are extra heartbeats, also known as ectopic beats, which can originate from one of the bottom of two heart chambers - atria or ventricles. Ectopic beats are also known as premature atrial contraction (PAC) or premature ventricular contraction (PVC). They are common, mostly harmless and may not cause any symptoms. Although typically not life-threatening, they would disrupt the regular heart rhythm. In majority of the cases, they may not require any treatment unless necessary, as advised by doctor based on the frequency of occurrence.
Atrial fibrillation (AF)/ flutter
This refer to an disorganised, rapid and irregular rhythm that originates from the atria. While it is not life-threatening, it is considered serious because it could create blood clots in the heart. Blood may pool in the left atrium and form clots which can block blood flow to the brain or other parts of the body. Patients with AF are at risk of stroke as well as heart failure.
Are arrhythmias common?
There have been numerous studies conducted globally to investigate the incidence and prevalence of arrhythmias. In a large-scale study comprising half a million community dwelling adults in the United Kingdom in 2018, the overall incidence of all these arrhythmias were 4.72 per 1,000 person years – which meant that for every 1,000 people followed up for one year, approximately five people would be newly diagnosed with any one of these arrhythmias1. As the current world population stands at 8 billion people, this translates to roughly 40 million new patients with newly diagnosed arrhythmias per year which is indeed a staggering number. Out of the many arrhythmias, the highest incidence was AF with an incidence of 3.11 per 1,000 person years in the same study.
AF is now the most common sustained arrhythmia with an estimated global prevalence of 46.3 million2. This is expected to increase with an aging population worldwide and better detection. In Asia, AF prevalence varies from 0.49 – 5.4% with a higher prevalence (4.6 – 8.2%) amongst those above 70 years of age3. Specific to Singapore, the AF prevalence was 1.5% in 20084 but this number has significantly increased since then. AF tends to affect more affluent and Western countries with Singapore having an intermediate prevalence rate (Figure 1)5.
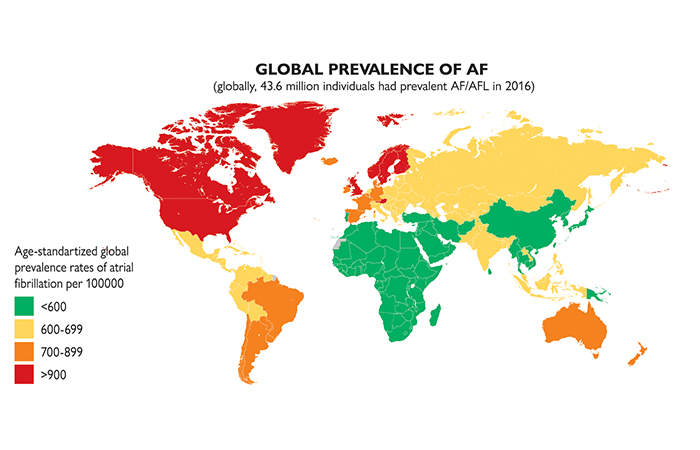
Figure 1: Global prevalence of AF (Source: 2020 ESC Guidelines for the diagnosis and management of atrial fibrillation)
Symptoms of arrhythmias
Patients with arrhythmias can either be asymptomatic (free of symptoms) or present with a myriad of symptoms.
Patients with tachycardia commonly experience palpitations or rapid heart rate but sometimes may occasionally experience breathlessness, chest tightness or infrequently fainting if episodes are prolonged. On the other hand, patients with bradycardia tend to feel breathlessness, exercise intolerance, light-headedness/ giddiness or have fainting spells.
Patients with premature or ectopic beats are mostly asymptomatic although some may experience the sensation of skipped beats from time to time.
On the other hand, patients with AF can have a broad range of symptoms encompassing all the above. However, in some cases, these symptoms may not be due to underlying heart disorders but instead may be either due to underlying pulmonary, neurological or psychogenic conditions. Thus, accurate history taking, examination and appropriate testing is crucial in diagnosing arrhythmias.
How do we diagnose/ detect arrhythmias?
Arrhythmia can generally be diagnosed with the use of heart rhythm tracings such as electrocardiogram (ECG) and Holter monitor. However, detection of arrhythmia remains a challenge as often times, an arrhythmia can occur suddenly and unpredictably, and resolve spontaneously within seconds to minutes. This poses challenges for physicians to be able to reliably capture and diagnose arrhythmia on monitoring devices. For instance, a patient who experienced symptoms suggestive of an arrhythmia and rushed to general practitioner (GP) or the emergency department (ED) to seek medical attention, but was told that the ECG was normal with no abnormality found.
Fortunately, with the advancement in technology, there have been an influx of newer digital heart rhythm or mobile health (mHealth) devices which are able to facilitate better detection of arrhythmias (Figure 2). The selection of devices for arrhythmia detection would depend on nature and frequency of symptoms as well as patients’ comfort and preference. It is also subject to the individual’s savviness in using such a device and navigating the functions. The use of mHealth devices have shown to be useful in some cases, especially in those with short bursts of arrhythmias that would have been missed otherwise using traditional detection method.
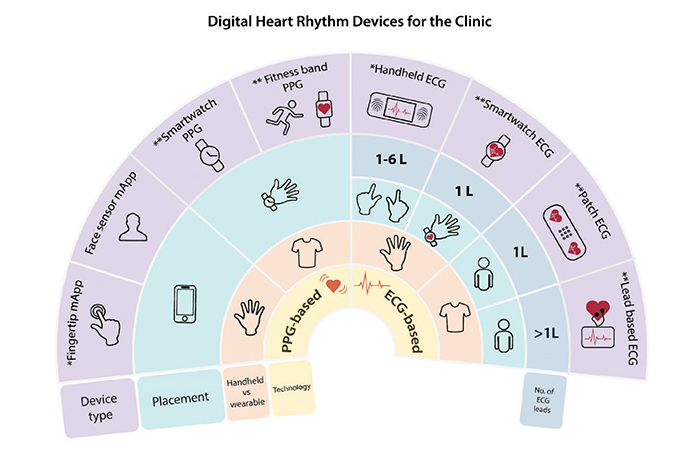
Figure 2: Array of digital heart rhythm devices for detection of arrhythmias (Source: How to use digital devices to detect and manage arrhythmias: an EHRA practical guide)
Treatment
Depending on the type of arrhythmia detected, your physician may recommend the following treatment options:
Vagal manoeuvres in SVT
A set of specific movement/ exercises that a person can carry out at home which can stop some type of arrhythmias.
Medications
While medications generally do not cure the arrhythmia, they can be useful in controlling number of episodes and improving symptoms.
In patients with AF, additional medications in the form of blood thinners (anticoagulants) may be required to prevent stroke.
Cardioversion
This uses electrical energy synchronised to one’s rhythm to urgently stop dangerous heart rhythms such as VT or in patients who are unstable/ ill.
Ablation therapy
The electrophysiologist inserts catheters inside the heart to confirm the nature of the arrhythmia following which energy (either heat/ cold source) will be applied to destroy the diseased segments of the heart to correct to arrhythmia.
Device therapies
Pacemakers – a small device that is usually implanted under the skin over the chest areas for those with irreversible bradycardias with abnormal rhythm.
Implantable cardio defibrillators – a slightly larger device than a pacemaker that is usually inserted in the same manner for those with known dangerous arrhythmias such as VT/VF or those with persistent heart muscle weakness (cardiomyopathies) despite treatment with medications.
If palpitations are accompanied by either severe chest pain, breathlessness, unusual profuse sweating or loss of onsciousness, one should seek medical condition immediately.
Prevention
Prevention is better than cure. Most heart disease prevention strategies can be divided into three main prongs – trigger avoidance, healthy lifestyle, and cardiovascular risk factor control. Arrhythmias are known to be associated with some triggers such as alcohol, physical or emotional stress as well as certain medications such as appetite suppressants. Complete abstinence may be impossible to some habitual alcohol drinkers, but one can continue to drink alcohol so long as it is in moderation. The Health Promotion Board (HPB) recommends no more than one drink a day for women and two drinks in a day for men – as heavy consumption or binge drinking has been shown to trigger arrhythmias. On the other hand, caffeinated beverages such as coffee and tea which used to be thought of as a trigger for arrhythmias, has since been debunked in numerous large studies and in fact been shown to be associated with lower incidence of arrhythmias6,7.
In terms of healthy lifestyle, having a balanced diet as per HPB recommendations, regular exercises and smoking avoidance can help to minimise cardiac diseases such as arrhythmias. It is recommended that individuals have at least 150 minutes of
moderate intensity aerobic exercises in a week to maintain general cardiorespiratory fitness. For those who are more sedentary or busy with work, they may find it challenging to achieve the 150 minutes of exercises, hence making some modifications to daily routines such as taking the stairs instead of the lift or trying to clock 10,000 steps can also be a form of exercise.
For those with known underlying cardiovascular risk factors such as diabetes, hypertension and hypercholesterolemia, good control of these conditions can reduce onset of arrhythmias as well.
1 Khurshid S, Choi SH, Weng LC, et al. Frequency of Cardiac Rhythm Abnormalities in a Half Million Adults. Circ Arrhythmia Electrophysiol. Published online 2018. doi:10.1161/CIRCEP.118.006273
2 Benjamin EJ, Muntner P, Alonso A, et al. Heart Disease and Stroke Statistics-2019 Update: A Report From the American Heart Association. Circulation. Published online 2019. doi:10.1161/ CIR.0000000000000659
3 Chan NY, Orchard J, Agbayani MJ, et al. 2021 Asia Pacific Heart Rhythm Society (APHRS) practice guidance on atrial fibrillation screening. J Arrhythmia. Published online 2022. doi:10.1002/ joa3.12669
4 Yap KB, Ng TP, Ong HY. Low prevalence of atrial fibrillation in community-dwelling Chinese aged 55 years or older in Singapore: a population-based study. J Electrocardiol. Published online 2008. doi:10.1016/j.jelectrocard.2007.03.012
5 Hindricks G, Potpara T, Dagres N, et al. 2020 ESC Guidelines for the diagnosis and management of atrial fibrillation developed in collaboration with the European Association for Cardio-Thoracic Surgery (EACTS). Eur Heart J. Published online 2021. doi:10.1093/eurheartj/ehaa612
6 Bodar V, Chen J, Gaziano JM, Albert C, Djoussé L. Coffee Consumption and Risk of Atrial Fibrillation in the Physicians’ Health Study. J Am Heart Assoc. Published online 2019. doi:10.1161/JAHA.118.011346
7 Kim E, Hoffmann TJ, Nah G, Vittinghoff E, Delling F, Marcus GM. Coffee Consumption and Incident Tachyarrhythmias. JAMA Intern Med. Published online 2021. doi:10.1001/jamainternmed.2021.3616
This
article is from Murmurs Issue 43 (May – August 2022). Click here to read other articles or issues.
