Ankle injuries, post-traumatic neck pain and lower back pain are commonly presented in primary care. Understanding the indications warranting further radiological investigations is crucial for effective management of these conditions.
INTRODUCTION
Ankle injury, neck injury and low back pain are common presentations in primary healthcare set-ups and can be managed satisfactorily in the outpatient setting. After history-taking and physical examination, primary care physicians have to decide whether further imaging is necessary in a given patient. The utilisation of radiological services is therefore an important part of our clinical practice at the Accident & Emergency Department (A&E).
For many clinicians, the indications for x-rays may have been largely learnt while on the job. Even though x-rays can be invaluable for the outlining of patient care, overuse can result in wastage of resources and unnecessary radiation exposure. Equally important is the need to understand the limitations of x-rays, so as not to develop a false sense of confidence and miss a diagnosis.
HOW TO DECIDE IF AN X-RAY IS NECESSARY
The points below summarise the guidelines which aid in deciding whether an x-ray is necessary for ankle injuries, cervical trauma and low back pain.
1. Ankle Injuries
The ankle is the second most commonly injured body part during sports. Ankle sprains constitute the majority of ankle injuries. The Ottawa Ankle Rules may help to determine if the patient requires x-rays and referral to the emergency department.
Ottawa Ankle Rules
Suitable patients for application of this rule include children two years old and above, and adults presenting with ankle injury. The original study included non-pregnant patients aged over 18 years with a new injury of less than 10 days old.
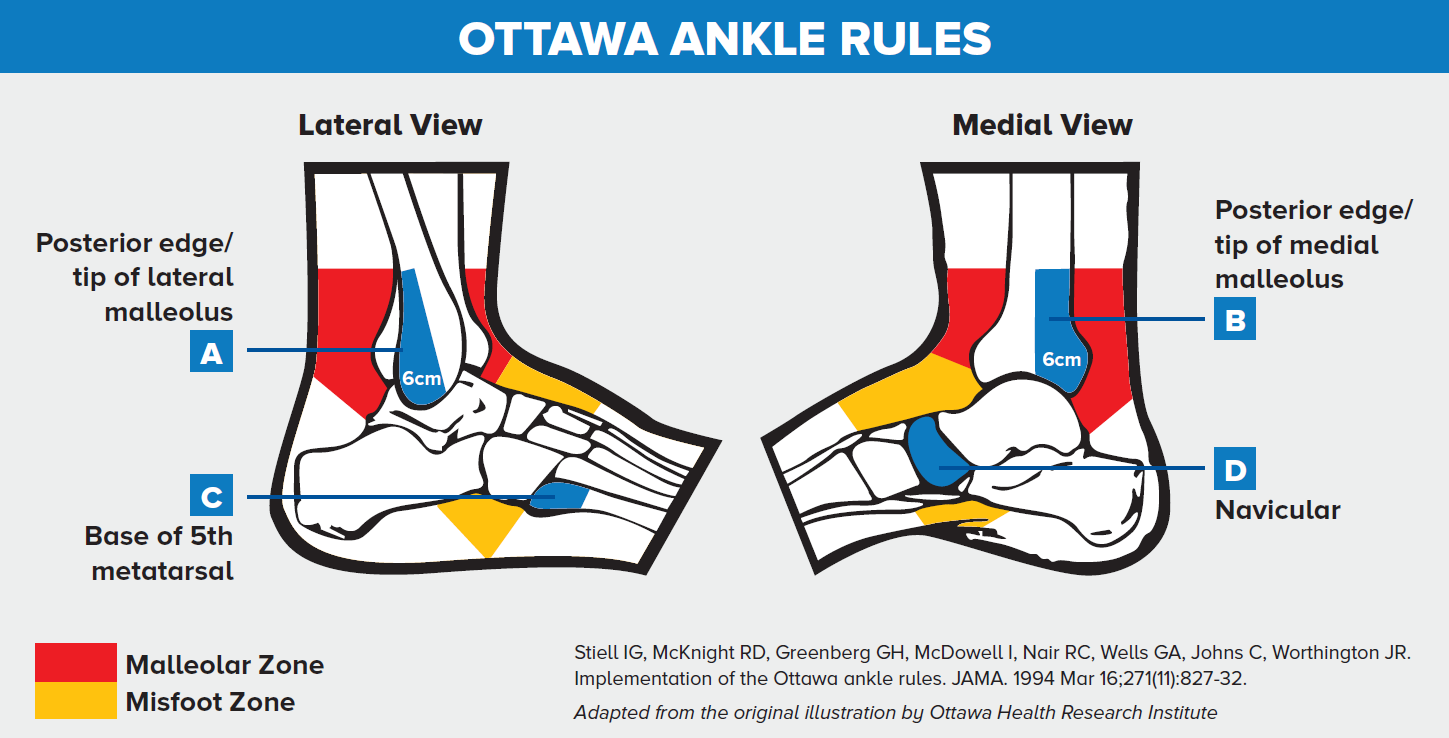
According to the Ottawa Ankle Rules, an ankle series of x-rays is only indicated for patients who have pain in the malleolar zone and:
- Have bony tenderness at the posterior edge or tip of the lateral and medial malleolus, or
- Are unable to bear weight both immediately after the injury and for four steps in the emergency department or doctor’s office
The following applies to the use of the Ottawa Ankle Rules:
- If the patient can transfer weight twice to each foot for four steps, he or she is considered able to bear weight, even if he or she limps
- Palpate the distal 6cm of the posterior edge of the fibula when assessing for bone tenderness
In the absence of the above findings, a patient with ankle sprain can be managed with rest, ice application, compression bandage, limb elevation and analgesia and with advice to return for review should their condition persist or worsen.
2. Post-traumatic Neck Pain
When evaluating a patient with traumatic injury, one of several clinical decisions that must be made is whether or not imaging of the cervical spine is indicated.
National Emergency X-Radiography Utilization Study Criteria
The National Emergency X-Radiography Utilization Study (NEXUS) criteria is one which helps to clear the cervical spine clinically. Imaging is not required if all the below criteria are satisfied:
- Normal level of alertness
- No posterior midline cervical tenderness
- No focal neurologic deficit
- No alcohol intoxication
- No distracting injury
The NEXUS criteria should be used with caution in elderly patients above 65 years old, due to lower sensitivity in this age group.
Once cleared by the NEXUS criteria, a neck sprain can be managed with analgesia, home physiotherapy exercises, patient reassurance, as well as posture and sleep position modifications.
Canadian C-Spine Rule
The other decision rule that can be used is the Canadian C-Spine Rule. This can be used to rule out cervical spine injury in alert and stable trauma patients without the need to obtain radiographic images.
Computed Tomography Scan Imaging
In the past, computed tomography (CT) scan imaging of the cervical spine was reserved for better clarification of injuries seen on screening x-ray exams, or in cases when adequate images could not be obtained via x-rays. Subsequently, there was a concern suggesting that x-rays were missing a significant number of injuries. Currently, CT scans are often preferred over plain radiographs of the cervical spine in emergency department patients with multiple injuries.
3. Low Back Pain
Low back pain affects two-thirds of adults during their lifetime and is the leading cause of work disability in the developed world.
However, only 5% of cases have serious underlying diseases or neurological symptoms requiring surgical treatment, and the aim of imaging is to pick up these 5% of patients. One needs to identify red flags in the history and physical examination to identify patients who need spinal imaging.
Some red flags (non-exhaustive) in low back pain patients are:
- Age < 20 or > 55 years
- History of spinal trauma or instrumentation
- Signs, symptoms or risk factors for infection like osteomyelitis
- History of recent cancer or risk factors for cancer
- Constant, progressive, non-mechanical pain
- Risk of vertebral compression fracture
- Neurological deficits, especially bladder or bowel symptoms
In the absence of red flags, it would often be reasonable to treat low back pain conservatively with analgesia and physiotherapy for four to six weeks before performing imaging, which in the first instance, would consist of the anterior-posterior (AP) and lateral views of the lumbar spine.
THE SINGHEALTH GPFIRST PROGRAMME
The SingHealth GPFirst programme encourages residents in the East and North-East to visit their GPs for mild to moderate medical conditions, rather than head to the emergency department at the first instance.
If found by participating GPs to require emergency care, patients who are referred to the CGH and SKH emergency departments will be accorded higher priority over P3 cases when they arrive at the A&E. In addition, they will receive a $50 subsidy on the prevailing A&E attendance fee.
GPFirst Participating Clinics are supported with:
- A&E Consultant Hotline (24/7)
- A&E Coordinator Hotline (during office hours)
- List of Exclusion Criteria (non-exhaustive)
- CME Online Asynchronous Learning (COAL) and quarterly CMEs
- GPFirst Aide Mobile App – with decision tools on 16 red-flag conditions
REFERENCES
- Stiell IG, Greenberg GH, McKnight RD, Nair RC, McDowell I, Reardon M, Stewart JP, Maloney J. Decision rules for the use of radiography in acute ankle injuries. Refinement and prospective validation. JAMA. 1993 Mar 3;269(9):1127-32. doi: 10.1001/jama.269.9.1127. PMID: 8433468.
- Hoffman JR, Mower WR, Wolfson AB, Todd KH, Zucker MI. Validity of a set of clinical criteria to rule out injury to the cervical spine in patients with blunt trauma. National Emergency X-Radiography Utilization Study Group. N Engl J Med. 2000 Jul 13;343(2):94-9. doi: 10.1056/NEJM200007133430203. Erratum in: N Engl J Med 2001 Feb 8;344(6):464. PMID: 10891516.
- Chou R, Qaseem A, Owens DK, Shekelle P; Clinical Guidelines Committee of the American College of Physicians. Diagnostic imaging for low back pain: advice for high-value health care from the American College of Physicians. Ann Intern Med. 2011 Feb 1;154(3):181-9. doi: 10.7326/0003-4819-154-3-201102010-00008. Erratum in: Ann Intern Med. 2012 Jan 3;156(1 Pt 1):71. PMID: 21282698.
Dr Rahalkar Kshitij, MBBS, MMed (Emergency Med), is a Senior Resident in the SingHealth Emergency Medicine Residency Programme, and currently works at Changi General Hospital.
Dr Lim Hoon Chin Steven, MBBS, MRCS A&E (Edin), FAMS, FCDMS, is Chief and Senior Consultant Emergency Physician at Changi General Hospital’s Accident & Emergency Department. He serves in the Society for Emergency Medicine in Singapore (SEMS) as Vice President. He is also the Vice Chairman (Clinical Services) of the SingHealth Emergency Medicine Academic Clinical Programme, and holds multiple academic and teaching appointments at local institutions. Dr Lim completed his Fellowship in Disaster Medicine at the University of California Irvine in the United States and is a member of the International Editorial Board of the Western Journal of Emergency Medicine.
Tags:
Ankle;Neck;Back
;
;
Ankle;Neck;Back;
;
News Article;
Changi General Hospital;
Changi General Hospital;
Article;
Defining Med;Medical News;
;
;
Changi General Hospital;Emergency Medicine;
;
Defining Med;Medical News (SingHealth);Patient Care
